- Donovanosis can cause painless, bright-red bumps and slowly enlarging genital sores that may bleed easily or develop foul-smelling drainage.
- Symptoms often appear gradually, from about 30 days up to 6 months after exposure, so early evaluation helps prevent spread and complications.
- Seek medical care promptly for genital ulcers or sores, especially if they’re growing, bleeding, producing pus, or accompanied by new pain or swelling.
Donovanosis is a chronic, progressive sexually transmitted infection (STI) caused by the bacterium Klebsiella granulomatis. It can cause painless, bright-red bumps and slowly enlarging sores or ulcers on the genitals, groin, or anus.
This condition is also called granuloma venereum or inguinal granuloma. It can affect men and women and is most often spread through unprotected vaginal, anal, or oral sex with someone who has the infection.
Donovanosis is treatable, and care is usually guided by a urologist (for men) or a gynecologist (for women). Treatment typically involves antibiotics to clear the bacteria and help the lesions heal.
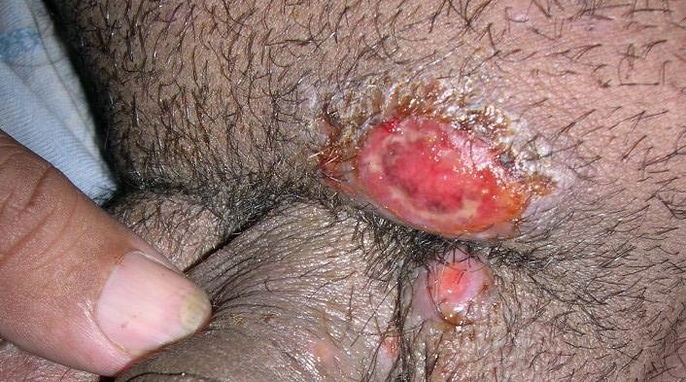
Main symptoms
The main symptoms of donovanosis are:
-
Bright-red bumps or nodules in the genital area that usually do not hurt;
-
Sores or ulcers that slowly get larger over time;
-
Lesions that bleed easily;
-
Discomfort where the lesions are located;
-
Foul-smelling drainage or pus if the lesions become infected.
In men, symptoms may appear on the foreskin, coronal sulcus, frenulum, glans, or scrotum. In women, symptoms may appear on the labia minora or labia majora, the vaginal opening, the cervix, or the upper genital tract.
Lesions can also occur in other areas, such as the anus, groin, face, lips, gums, pharynx, larynx, or chest.
If the infection is not treated, it can spread to internal organs such as the lungs, liver, spleen, joints, or bones.
When do symptoms appear?
Symptoms of donovanosis usually develop gradually over time. They often appear about 30 days to 6 months after contact with the bacteria.
It’s important to see a urologist or gynecologist if you notice possible symptoms of donovanosis. This helps ensure the right diagnosis and early treatment.
Confirming a diagnosis
Donovanosis is diagnosed by a urologist, gynecologist, or infectious disease specialist. Diagnosis is based on symptoms, a physical exam of the genital area, lifestyle habits, medical history, and any history of unprotected sexual contact.
The doctor may also take a fluid sample from a sore or ulcer to test for Klebsiella granulomatis. According to the Centers for Disease Control and Prevention (CDC), a diagnosis of donovanosis is confirmed by identifying characteristic findings in tissue or biopsy samples, since the organism is difficult to grow in culture.
These tests can confirm donovanosis and help rule out other conditions with similar symptoms, such as syphilis, chancroid, lymphogranuloma venereum, or cancer.
Testing for other STIs may also be recommended, especially an HIV test.
Donovanosis and HIV
Because donovanosis causes open sores, it increases the risk of other infections entering the body. This makes people with donovanosis more likely to acquire HIV.
Transmission and spread
Donovanosis is mainly spread through unprotected vaginal, anal, or oral sex, meaning sex without a condom.
Although rare, it may also spread through non-sexual contact, such as fecal transmission, or during vaginal childbirth.
Treatment options
Treatment should be guided by a urologist, gynecologist, or infectious disease specialist. Antibiotics are usually recommended to eliminate the bacteria, treat the infection, support healing, and help prevent secondary infections.
The main treatments for donovanosis are:
1. Antibiotics
The main antibiotics a doctor may recommend include:
-
Erythromycin;
-
Sulfamethoxazole and trimethoprim.
Antibiotics are usually taken for at least three weeks and continued until all genital sores have completely healed, following CDC STI Treatment Guidelines.
If symptoms don’t begin to improve within the first few days, you should return to your doctor. Your provider may consider adding another antibiotic, often an aminoglycoside such as gentamicin, to help the infection clear.
2. Surgery
If lesions are extensive, surgical removal of the lesion may be recommended.
Surgery does not cure the infection on its own, so antibiotics still need to be taken as directed.
3. Regular medical follow-up
During and after treatment, it’s important to keep regular follow-up appointments and complete any recommended testing.
This helps your doctor track your response to treatment and confirm the bacteria are being eliminated. If needed, the antibiotic can be changed.
4. Self-care
Along with taking antibiotics as prescribed, these steps can support recovery:
-
Take treatment exactly as prescribed and for the full time recommended;
-
Keep the genital area clean to reduce the chance of infection and support healing;
-
Avoid sexual contact until the infection is fully cured;
-
Do not stop treatment on your own.
If you had sexual contact within the 60 days before your diagnosis, it's important to inform your partner so they can see a doctor for evaluation and begin treatment if necessary.
Is donovanosis curable?
Donovanosis can be cured when treatment is followed exactly as prescribed.
Possible complications
Donovanosis can lead to complications if it spreads to internal organs. This may result in conditions such as osteomyelitis or polyarthritis.
Other possible complications include vaginal bleeding, narrowing of the vaginal canal, anal canal, or urethra, scarring on the penis or scrotum, and cancer.
Prevention measures
To help prevent donovanosis, it is recommended to:
-
Use a condom during all sexual activity, including vaginal, anal, and oral sex;
-
Avoid sexual contact while symptoms are present;
-
Get regular testing for STIs;
-
Reduce STI risk by limiting the number of sexual partners.
Doing regular self-checks of the genitals and watching for changes in odor, color, appearance, or skin can help you notice problems earlier. This can lead to faster evaluation and treatment.






























