Hemoglobin in the urine, also called hemoglobinuria, occurs when red blood cells break down and release hemoglobin into the bloodstream, which then passes into the urine. This can cause the urine to appear reddish or unusually transparent and may be associated with conditions such as kidney infections, severe burns, malaria, or certain blood disorders.
A positive result does not always reveal the exact cause. Urine tests can detect signs of blood or related abnormalities but cannot show their source, so additional testing is often needed to determine the underlying reason.
Hemoglobin in the urine can appear in children, adults, and pregnant individuals, and may sometimes occur together with visible blood. Common causes include kidney infections, hemolytic anemia, malaria, transfusion reactions, renal tuberculosis, and other conditions that require prompt medical attention.
Main causes
The presence of hemoglobin in the urine may be caused by:
1. Kidney infection
A severe kidney infection, such as acute nephritis, nephritic syndrome, or pyelonephritis, can cause hemoglobin in the urine.
This usually occurs when red blood cells leak into the urine as a result of kidney inflammation or injury, rather than from widespread destruction of red blood cells within the blood vessels.
The most common symptoms of a kidney infection include cloudy or bloody urine, pain or burning with urination (dysuria), fever, back or flank pain, and feeling generally unwell.
What to do: If these symptoms appear, you should see a doctor right away to start the proper treatment.
The doctor may prescribe antibiotics and, in some cases, recommend hospitalization for IV medications.
2. Severe burns
In people with severe burns, hemoglobin may appear in the urine because extreme heat destroys red blood cells, releasing hemoglobin into the bloodstream.
When there is also muscle damage, such as with extensive burns or electrical burns, myoglobin is released as well.
These proteins reach the kidneys and are filtered into the urine, where they can build up and block the kidney tubules, increasing the risk of kidney damage and acute kidney failure if not treated in time.
What to do: In cases of severe burns, it is essential to go to or call emergency services immediately so treatment can begin as quickly as possible.
3. Hemolytic anemia
Hemolytic anemia is a condition in which red blood cells are destroyed faster than the body can replace them.
When blood hemoglobin levels are elevated, excess hemoglobin is filtered by the kidneys and excreted in the urine. This can cause the urine to appear dark, particularly in the first morning sample or during periods of active hemolysis.
This process may happen along with symptoms such as severe fatigue, paleness, yellowing of the skin and eyes, shortness of breath, and general malaise.
What to do: If symptoms suggest hemolytic anemia, it is important to see a doctor to confirm the diagnosis, identify the cause, and begin the right treatment to prevent complications.
4. Malaria
Malaria is an infection caused by parasites from the Plasmodium genus that invade and rupture red blood cells. This breakdown releases hemoglobin into the urine, making it look dark or reddish.
According to the World Health Organization (WHO), malaria commonly causes fever, chills, and fatigue, and it requires prompt diagnosis and treatment to help prevent serious complications.
What to do: It is essential to see a healthcare provider right away for evaluation and treatment to eliminate the parasite and prevent serious complications.
It is also recommended to stay well hydrated, avoid alcohol, and maintain a healthy diet.
5. Reaction to a blood transfusion
Hemoglobin in the urine may occur after a blood transfusion because of an incompatibility between the donor’s blood and the recipient’s blood. This is known as an acute hemolytic transfusion reaction.
When the transfused red blood cells are attacked and destroyed inside the blood vessels, hemoglobin is released into the bloodstream.
If there is too much hemoglobin, the kidneys filter it and pass it into the urine, which may then look dark or reddish.
This process may also cause dark or red urine, fever, chills, abdominal or back pain, and, in severe cases, acute kidney failure, shock, or disseminated intravascular coagulation (DIC).
What to do: This reaction can happen within the first few hours after a transfusion. Anyone who is still in the hospital should tell the medical team immediately if these symptoms appear.
6. Renal tuberculosis
Renal tuberculosis is an infection caused by the bacterium Mycobacterium tuberculosis that affects the kidneys and other parts of the urinary tract.
This disease may lead to hemoglobin being detected in the urine, although in reality the finding is often whole blood, called hematuria, rather than free hemoglobin.
The damage caused by the bacteria to the kidney and urinary tract tissues leads to bleeding, which is detected on urine testing.
Urine test strips may show positive hemoglobin, but when the sample is examined under a microscope, intact red blood cells are seen, sometimes in large numbers.
What to do: If a urine test shows blood or hemoglobin, the doctor will usually order additional tests to confirm the cause, such as microscopic urine analysis, cultures for Mycobacterium tuberculosis, and imaging tests of the urinary tract.
This helps confirm the diagnosis and allows the right treatment to begin.
7. Paroxysmal nocturnal hemoglobinuria
Paroxysmal nocturnal hemoglobinuria is a rare blood disorder in which red blood cells are destroyed inside the blood vessels, releasing hemoglobin into the urine.
This happens because the red blood cells lack certain proteins that normally protect them from the immune system, making them more vulnerable to damage.
People with this condition may have severe fatigue and notice dark or reddish urine, especially with the first morning urine.
What to do: It is important to keep regular medical appointments, because this condition can lead to serious complications and requires specialized monitoring and treatment.
8. Menstruation
Menstruation does not cause free hemoglobin in the blood, but it can cause a positive urine result for hemoglobin because of outside contamination.
During menstruation, blood can mix with urine during sample collection. Since urine test strips do not distinguish between free hemoglobin, blood from the urinary tract, and outside contamination, they may show a positive result for blood.
What to do: To help avoid false-positive results, it is recommended to wash the genital area well before collecting the sample and collect a midstream urine sample.
If possible, it is also recommended to wait until the menstrual period has ended or to use an appropriate tampon during collection.
9. Hemolytic uremic syndrome
Hemolytic uremic syndrome (HUS) is a severe illness most often triggered by infection with Escherichia coli (E. coli) bacteria, which can contaminate foods such as meat and vegetables.
According to the CDC, HUS is a serious complication of Shiga toxin-producing E. coli infection that may result in kidney failure, long-term health issues, or even death. The condition damages small blood vessels, particularly in the kidneys, leading to anemia, clotting abnormalities, high blood pressure, fatigue, and decreased urine output.
A person may have a positive result for hemoglobin in the urine because damage to the kidney blood vessels allows red blood cells to pass into the urine.
In addition, red blood cells may break apart while passing through blood vessels that are partly blocked by microthrombi, releasing hemoglobin that also ends up in the urine.
What to do: It is important to see a doctor immediately to start treatment as soon as possible and prevent complications, because this is a serious condition that affects both the blood and the kidneys.
Is hemoglobin in the urine serious?
The presence of hemoglobin in the urine can be an important finding, but it is not always serious.
This is because rapid urine tests do not identify where the blood is coming from and may be positive because of free hemoglobin, intact red blood cells, or contamination of the sample.
For that reason, a positive hemoglobin result by itself does not identify the exact cause and usually needs follow-up testing.
In many cases, the underlying cause can be treated, and a thorough medical evaluation can help identify its source and determine whether treatment is necessary.
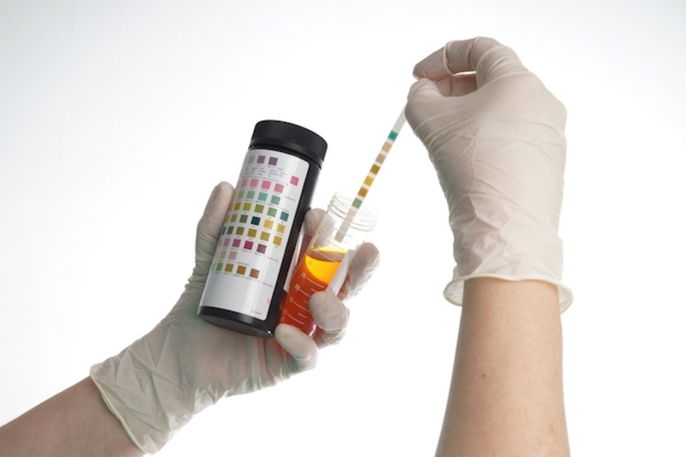
How it's detected
Hemoglobin in urine is considered positive when a reagent test strip changes color after the chemical reaction. It is considered negative when the strip shows no color change.
In general, a darker color change on the test strip indicates a higher amount of blood in the urine. However, it is important to read the instructions on the reagent strip package, since interpretation can vary by laboratory.
In addition to the rapid test, a microscopic exam may also be done by analyzing urinary sediment, which detects how much blood is present. In this case, having fewer than 3 to 5 red blood cells per field or fewer than 5,000 cells per mL is usually considered normal.
Traces of hemoglobin in the urine
Traces of hemoglobin in the urine indicate the presence of a very small, barely detectable amount of blood that should not normally be present.
Traces of hemoglobin are identified with a reagent strip and may represent intact red blood cells, free hemoglobin, or even sample contamination, since the test does not identify the source.
For that reason, the presence of trace hemoglobin alone is not enough to make a diagnosis; it’s a finding that usually requires confirmation with additional tests.
Signs and symptoms
Hemoglobin in the urine doesn’t cause symptoms on its own. When symptoms do occur, they are usually due to the underlying condition responsible for the presence of hemoglobin.
However, urine color may change and may look red and clear. In severe cases, the loss of a large amount of hemoglobin may also cause fatigue, paleness, and even anemia.






























