- Sepsis is a medical emergency where an infection triggers a dangerous body-wide response, often causing fever (or low temperature), rapid breathing, fast heart rate, confusion, low blood pressure, and very low urine output.
- Risk is higher in babies, adults 65+, and people with chronic illness or weakened immunity, and sepsis can start from common infections like pneumonia, UTIs, or skin infections.
- Seek emergency care immediately if sepsis is suspected, especially when infection symptoms come with confusion, trouble breathing, faintness/very low blood pressure, or a sudden worsening in how someone looks or acts.
Sepsis is the body’s extreme response to an infection caused by bacteria, fungi, or viruses. It can lead to low blood pressure, fever, a fast heart rate, shortness of breath, and confusion.
Sepsis can affect anyone, but it most often occurs in people with weakened immune systems. This includes newborns, adults over age 65, and people with chronic conditions such as diabetes, lung disease, or kidney disease.
If you think someone may have sepsis, go to the hospital right away. A clinician can confirm the diagnosis and start treatment as soon as possible.
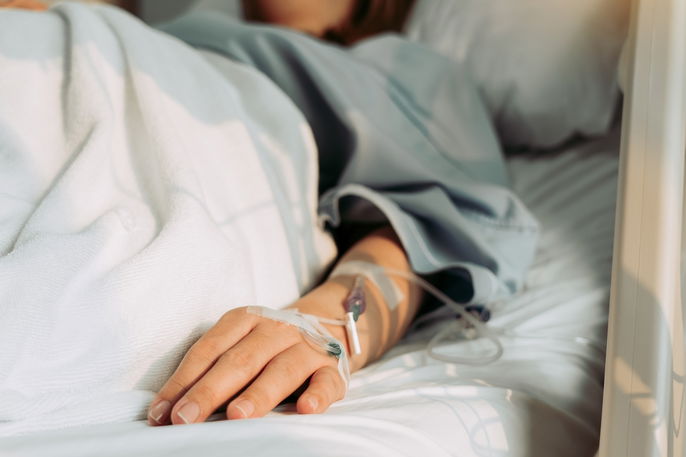
Main symptoms
The main symptoms and signs of sepsis are:
-
Increased heart rate;
-
Shortness of breath or rapid breathing;
-
Fever or low body temperature;
-
Confusion or agitation;
-
Decreased urine output;
-
Severe fatigue.
When sepsis is not recognized early and managed promptly, it can progress to septic shock and death, according to the World Health Organization (WHO).
Different types
The main types of sepsis are classified according to the type of infection that triggers them. These include:
1. Pulmonary sepsis
Pulmonary sepsis happens when the infection is in the lungs and, in most cases, is linked to pneumonia caused by bacteria, especially Streptococcus pneumoniae.
Even though the infection starts in the lungs, inflammation can spread throughout the body, causing fever, chills, muscle aches, and breathing changes such as rapid breathing, shortness of breath, and severe fatigue.
2. Neonatal sepsis
Neonatal sepsis is an infection that affects the bloodstream in newborns younger than 28 days old and occurs most often in premature babies, since their immune systems are less developed.
This type of sepsis may occur when microorganisms are transmitted from the mother’s vagina or uterus to the baby, or through contact with healthcare workers or caregivers.
3. Urinary sepsis
Urinary sepsis, also called urosepsis, is a body-wide inflammatory response to urinary tract infections (UTIs), such as cystitis, pyelonephritis, and prostatitis.
Symptoms of urinary sepsis vary depending on the condition that caused it and may include painful urination (dysuria), blood in the urine, fever, lower abdominal pain, and feeling unwell.
4. Abdominal sepsis
Abdominal sepsis can be caused by infections such as appendicitis, peritonitis, biliary infection, or liver infection, and may lead to symptoms such as abdominal pain, fever, loss of appetite, nausea, vomiting, and abdominal swelling.
5. Cutaneous sepsis
Cutaneous sepsis can occur when bacteria reach deeper layers of the skin, such as in necrotizing fasciitis, infectious cellulitis, ecthyma, diabetic foot infections, and pressure ulcers, for example.
Symptoms of cutaneous sepsis may include fever, darkening of the affected area, pain, swelling, skin redness, pus, and swollen lymph nodes.
Confirming a diagnosis
Sepsis must be diagnosed in a hospital by evaluating the person’s symptoms and signs and reviewing their health history.
To confirm the diagnosis, a clinician may order lab and imaging tests such as blood cultures, a urine test, a complete blood count (CBC), an X-ray, and a computed tomography (CT) scan, for example.
A clinician may also use the Sequential Organ Failure Assessment, which estimates sepsis risk based on having at least two of the following: systolic blood pressure below 100 mmHg, breathing rate above 22 breaths per minute, and a score of 15 or less on the Glasgow Coma Scale (used to assess level of consciousness).
Possible causes
Sepsis can develop from an untreated infection caused by bacteria, fungi, or viruses, such as a urinary tract infection (UTI), intestinal infection, pneumonia, or infectious cellulitis, for example.
According to the Centers for Disease Control and Prevention (CDC), adults 65 or older, infants, people with chronic conditions (such as diabetes and lung disease), and people with weakened immune systems are at higher risk of developing sepsis.
Treatment options
Treatment for sepsis should start as quickly as possible in the hospital and may include:
-
Antibiotics, given directly into a vein, for infections caused by bacteria;
-
Intravenous (IV) fluids, given through an IV, to maintain adequate blood flow and help prevent a severe drop in blood pressure;
-
Vasopressor medications, such as norepinephrine, vasopressin, and dopamine, to raise blood pressure;
-
Dialysis, which may be recommended in cases of kidney failure.
In some cases, surgery may also be recommended to remove tissue damaged by the infection.
Is sepsis curable?
Sepsis can be cured, but because it can lead to serious complications, it should be treated as soon as possible to reduce the risk of septic shock. Early diagnosis and prompt treatment improve the chances of recovery.
Prevention measures
The main ways to help prevent sepsis are:
-
Keeping cuts and wounds clean;
-
Staying up to date on recommended vaccines;
-
Washing your hands well before preparing food and eating; after using the bathroom, blowing your nose, or coughing; and after touching animals;
-
Maintaining a healthy diet;
-
Breastfeeding a baby for at least the first 6 months of life.
Another way to help prevent sepsis is to manage chronic conditions effectively by following your clinician’s recommended treatment plan.






























