- Rapid growth, new raised texture, or a blue nevus larger than usual should be evaluated, especially if it changes over weeks to months.
- Irregular borders, asymmetry, or color changes can signal a concerning skin change and warrant a dermatology exam.
- Itching, pain, bleeding, or a sore that keeps returning are warning signs that should not be ignored.
Blue nevus is a type of skin lesion caused by a buildup of melanocytes, the cells that make melanin. It often looks like a blue-to-black spot or bump on the skin.
Most people have just one blue nevus. Some people can develop several lesions grouped together, and this may be linked to congenital or acquired factors.
A dermatologist determines the treatment approach based on the characteristics of the lesion, which may involve regular monitoring or surgical removal.
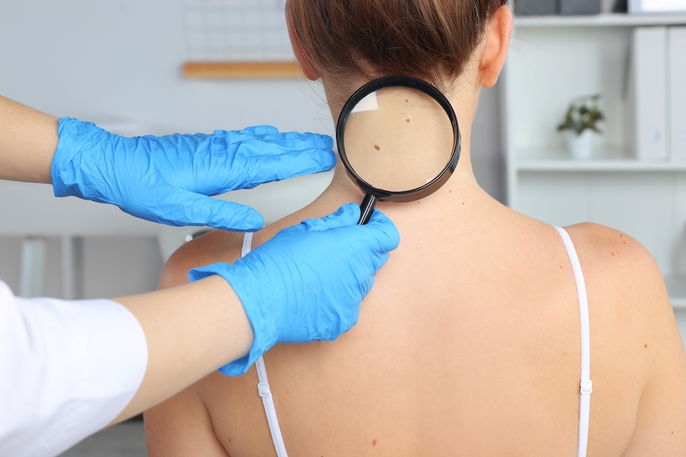
Common symptoms
The main symptoms of a blue nevus are:
-
Blue, dark gray, brown, yellowish, or black spot on the skin;
-
Round shape;
-
Size between 1 and 5 mm;
-
Flat or raised spot or plaque, similar to a wart.
A blue nevus most often appears on the scalp, neck, face, lower back, hands or feet, or buttocks.
It is important to see a dermatologist to evaluate the skin, confirm the type of blue nevus, and decide whether treatment is needed.
Is a blue nevus cancer?
In most cases, a blue nevus is a harmless skin lesion that does not pose any health risk. For this reason, removal is usually unnecessary.
In some cases, malignant cells can develop in the area. This is more likely when the blue nevus is very large or grows quickly.
Also recommended: Signs of Skin Cancer (Melanoma & Nonmelanoma) tuasaude.com/en/signs-of-skin-cancerConfirming a diagnosis
Diagnosing a blue nevus is usually straightforward. A dermatologist can often identify it by examining the lesion’s appearance.
To support the diagnosis, the doctor may use dermoscopy, which provides a closer, more detailed view of the lesion.
If the diagnosis is unclear, the doctor may do a biopsy of the blue nevus to rule out other conditions that can look similar, such as dermatofibroma, melanoma, or Kaposi sarcoma.
Possible causes
The exact cause of blue nevus is not fully known. It is linked to the buildup and growth of melanocytes, which make melanin, the pigment that gives skin its color.
Because these cells sit deeper in the skin, the pigment is not seen in the usual way. This can make the lesion appear blue, sometimes ranging to dark gray.
One theory is that blue nevi are related to incomplete migration of melanocytes from the neural crest during fetal development.
Another theory is that it starts from specific stem cells within the dermis.
Main types
The main types of blue nevus are:
1. Common blue nevus
This is the most common type. It is usually small (typically less than 0.5 cm) and often appears on the hands or feet. It may occur as a single lesion or as multiple ones.
2. Cellular blue nevus
This is a variant of the common blue nevus and is usually larger, around 1 to 3 cm. It more often appears on the buttocks and sacral area, on the lower back.
Cellular blue nevus is more common in women and may have an uneven surface. Because of this, it can be mistaken for melanoma on a skin exam and on diagnostic testing.
3. Amelanotic blue nevus
Amelanotic blue nevus has little or no melanin pigment. It is caused by the growth of spindle-shaped cells in the skin.
4. Malignant blue nevus
Malignant blue nevus is rare, but it is considered a variant of melanoma and is usually associated with cellular blue nevus. It tends to grow quickly and may form lesions larger than 3 cm with an irregular surface.
Treatment options
Treatment should be guided by a dermatologist and depends on the lesion’s characteristics.
If the blue nevus is stable, meaning it is not growing, the doctor may recommend regular follow-up visits. This helps check whether it increases in size or changes in appearance.
If the blue nevus grows, or if it is a cellular blue nevus or malignant blue nevus, surgery is recommended.
This procedure can be done in the dermatologist’s office with local anesthesia, and no special preparation is usually needed. The blue nevus is typically removed in about 20 minutes and then sent to a lab to check for malignant cells.
In some cases, a second procedure may be recommended to remove a small amount of surrounding tissue. This is done to help ensure all cancerous cells are removed.
When to see a doctor
It is recommended to see a dermatologist if:
-
The nevus increases rapidly in size;
-
It develops an irregular border;
-
There are changes in color or multiple colors appear;
-
The spot is asymmetrical;
-
The nevus begins to itch, hurt, or bleed.
In these situations, the doctor should evaluate whether the lesion is benign or malignant and recommend the most appropriate treatment.
The American Cancer Society notes that a new spot or a spot that changes in size, shape, or color can be an important warning sign for melanoma.






























