Frostbite causes symptoms such as skin redness, and the skin may also look gray or whitish. The area may feel numb or tingly, blisters may form, and any part of the body that has touched ice can be affected.
This type of burn can happen when the skin stays in direct contact with ice for too long. It is more common when ice packs are applied directly to the skin without a protective layer and for an extended period, but it can also happen after prolonged exposure to freezing temperatures and cold wind.
Frostbite can often be treated at home by moving to a warm place or placing the affected area in warm water. However, if the skin becomes hard or dark, numbness occurs, or the injury affects children or older adults, it is recommended to go to the emergency room right away.
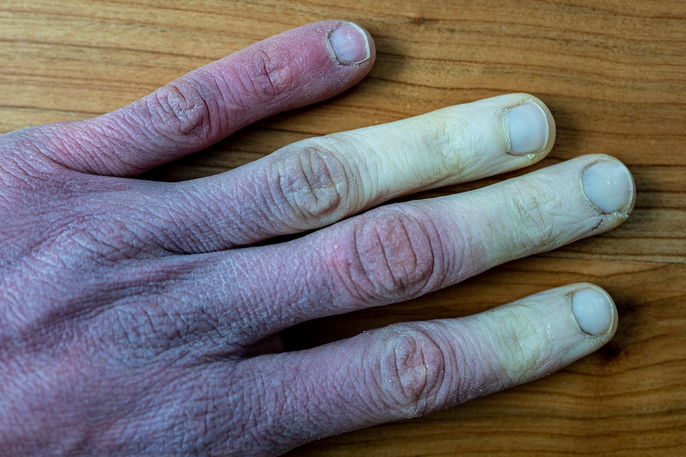
Symptoms of frostbite
The main symptoms of frostbite are:
-
Bright red, white, yellow, or grayish skin
-
Pain in the affected area
-
Numbness or tingling
-
Itching in the area
The symptoms of frostbite are usually very similar to first-degree sunburn, when only the epidermis is affected. The epidermis is the outermost and most superficial layer of the skin.
However, in more severe cases, blisters may also appear on the skin, as can happen with second-degree burns. The affected skin may also become hard and dark. According to the American Academy of Dermatology Association, emergency care is recommended if feeling does not return to the affected area or if the skin begins to turn gray.
How does ice burn skin?
When the skin stays in contact with ice for too long, the local blood vessels narrow. This reduces the flow of blood and nutrients to the area, causing cell damage.
In addition, prolonged skin exposure to ice causes skin cells to freeze. This can lead to tissue damage and cell death.
The longer the skin is exposed to ice, the greater the damage can be. For example, the injury may reach deeper layers of the skin or even the muscles.
Does frostbite leave a scar?
Frostbite can leave a scar on the skin. The scar may be permanent if the injury affects deeper layers of the skin or even the muscles, due to cell damage caused by prolonged exposure to ice.
What to do for frostbite
When frostbite occurs, the recommended first aid steps are:
-
Remove the ice from the skin immediately and, if clothing has become wet or cold, remove it as well
-
Soak the affected area in warm water, between 98.6ºF and 102.2ºF, for 20 minutes, or take a warm bath. If the skin still feels cold or numb, the affected area can be soaked in warm water for another 20 minutes, with at least 20 minutes between each soak
-
Move to a warm place and cover the skin with layers of clothing or a blanket
-
Apply warm compresses to the area for 20 minutes if there is no improvement after soaking the area in warm water
-
Do not rub or massage frostbitten skin, as this can cause more skin damage
In addition, it is important to drink more water, cover the skin with sterile gauze to help protect against infection, or apply a moisturizing lotion if the skin is intact, meaning there are no wounds or blisters.
When soaking the skin in warm water, make sure the water is not too hot, as this can make the burn worse. According to the Centers for Disease Control and Prevention, frostbitten areas should be warmed in warm, not hot, water, and direct heat sources such as a heating pad, heat lamp, stove, fireplace, or radiator should be avoided because numb skin can burn easily.
Main causes of frostbite
Frostbite can happen when ice stays in contact with the skin for too long. It is very common after ice packs are applied directly to the skin without a protective layer and for too long.
These burns can happen on any part of the body that stays in contact with ice for an extended period. For example, they can affect the face or lips after using ice packs following a tooth extraction, or they can affect joints when ice is used to relieve pain and swelling after an injury.
In addition, frostbite can also happen after prolonged contact with snow, very low temperatures, or very cold wind.
Some factors can also increase the risk of frostbite, such as smoking, diabetes, vascular disease, peripheral neuropathy, or the use of medications that lower blood pressure, for example.
When to see a doctor
It is important to go to the emergency room in the following cases:
-
Skin that remains hard, cold, or numb even after warming
-
Worsening symptoms or darkening of the skin
-
Blisters on the skin, which may contain pus or green fluid
-
Cracks, wounds, or ulcers on the skin
-
Fever
-
Severe pain in the area
For babies, children, or older adults, you should always go to the emergency room, regardless of the size of the burn or the intensity of the symptoms.
In addition, if the burn affects the face, lips, neck, palms of the hands, soles of the feet, wrist, buttocks, or knees, it is important to go to the emergency room immediately. These areas have a higher risk of infection.
Treatment options
Treatment for severe frostbite is done in the hospital by a general practitioner. It involves warming the affected area and using pain relievers to relieve pain.
In addition, the doctor may recommend antibiotics if there are signs of a bacterial infection in the affected area. The doctor may also use IV medication to improve blood flow.
If gangrene occurs, which is tissue death, the doctor may perform a procedure called debridement. This procedure removes dead and infected tissue from the skin to improve healing and help prevent the infection from spreading to other parts of the body.
- Frostbite can cause red, pale, grayish, numb, or blistered skin after prolonged contact with ice, freezing temperatures, or cold wind.
- First aid includes removing the ice, warming the affected area in warm water, covering the skin, and avoiding rubbing or massaging the area.
- Emergency care is recommended if the skin becomes hard or dark, symptoms worsen, blisters appear, or frostbite affects babies, children, or older adults.






























