Dermatitis herpetiformis is a chronic autoimmune disease that causes small red blisters on the skin. These blisters may cluster together, cause intense itching, and look similar to lesions caused by herpes.
It most often affects the scalp, shoulders, buttocks, elbows, and knees. This condition is also known as Duhring-Brocq disease or celiac dermatitis herpetiformis.
Dermatitis herpetiformis is more common in people with celiac disease because it appears to be related to sensitivity to gluten, a protein found in rye, wheat, malt, and barley. Treatment is guided by a dermatologist or primary care provider and usually includes removing gluten from the diet and using medications to help relieve symptoms.
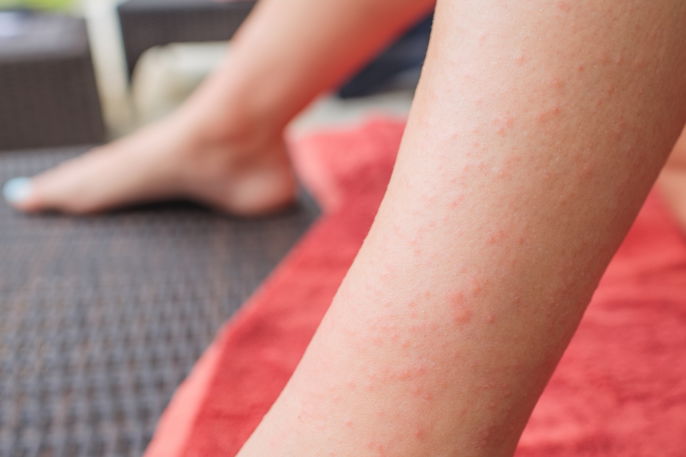
Main symptoms
The main symptoms of dermatitis herpetiformis are:
-
Grouped red blisters on the skin
-
Flat red patches
-
Itching on the back, scalp, shoulders, buttocks, elbows, or knees
-
A burning sensation in the affected areas
-
Blisters that break easily when scratched
-
Red plaques or welts with scaling
-
Sores around the blisters
Symptoms of dermatitis herpetiformis commonly appear on the scalp, buttocks, elbows, knees, and back. They usually appear symmetrically, meaning they affect both elbows or both knees, for example.
In general, dermatitis herpetiformis does not leave scars after the lesions go away. However, it may leave lighter or darker spots on the skin.
Symptom test
Dermatitis herpetiformis is a type of dermatitis, similar to contact dermatitis and atopic dermatitis. To see whether your symptoms may be related to dermatitis, please select the symptoms you are experiencing below:
This test is only a tool. It is not meant to provide a diagnosis or replace an appointment with a dermatologist or your primary care provider.
Confirming a diagnosis
Dermatitis herpetiformis is diagnosed by a dermatologist or primary care provider based on the appearance of the skin lesions and the person’s medical history.
To confirm the diagnosis, the provider should order a skin biopsy, in which a small sample of the affected skin is removed and examined in a laboratory.
According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), this testing can confirm dermatitis herpetiformis by identifying immunoglobulin A (IgA) deposits that are typically seen with this condition.
In addition, the provider may order tests for celiac disease, such as urine, stool, and blood tests to check antibody levels, as well as genetic testing and intestinal endoscopy with biopsy, for example.
Possible causes
The main cause of dermatitis herpetiformis is gluten intolerance. This substance can activate the immune system and lead to the formation of immunoglobulin A (IgA), which causes the body to attack cells in the intestines and skin.
Genetic predisposition, such as having a first-degree relative like a parent with celiac disease or dermatitis herpetiformis, appears to increase the risk of developing these conditions.
In addition, exposure to iodine also appears to increase the risk of dermatitis herpetiformis flare-ups in people with celiac disease.
Treatment options
Treatment for dermatitis herpetiformis should be guided by a dermatologist or primary care provider based on the characteristics of the blisters and the other symptoms present.
A strict gluten-free diet is recommended first to help prevent new blisters. According to the NIDDK, dermatitis herpetiformis is gluten-sensitive, and while a gluten-free diet treats the underlying condition, the skin symptoms may still take months to fully improve.
Because the diet can take some time to work, the dermatologist may also recommend an oral antibiotic such as dapsone, which can relieve symptoms within 1 to 3 days.
Dapsone can cause side effects such as diarrhea, nausea, and anemia, so the dose is usually adjusted over time to find the lowest amount that still controls symptoms.
For people who cannot tolerate dapsone, the dermatologist may prescribe corticosteroid ointments or another medicine, such as sulfasalazine, for example.






























