Hidradenitis suppurativa is a chronic inflammatory skin condition that primarily affects the hair follicles. This condition leads to painful lumps under the skin that may rupture and cause significant scarring.
Commonly known as acne inversa, this condition typically develops in areas where skin rubs together. You will most often find these painful nodules in the armpits, groin, buttocks, or under the breasts.
While a permanent cure does not currently exist, various medical treatments can help manage the symptoms effectively. Dermatologists often use a combination of medications and surgical procedures to prevent the condition from worsening.
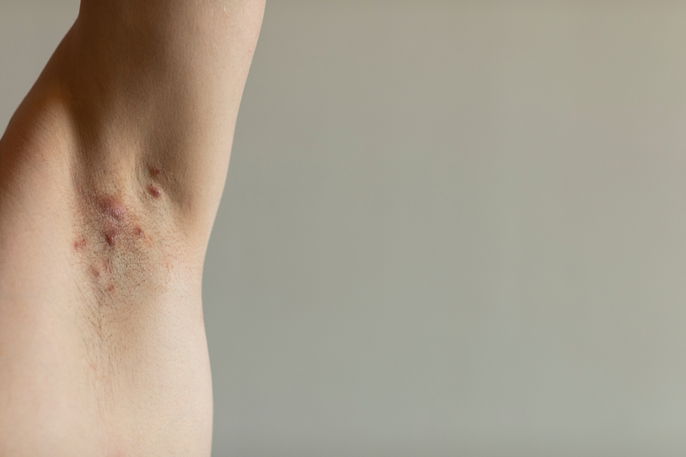
Main symptoms
The primary symptoms of hidradenitis suppurativa include:
-
Hard lumps or pus-filled nodules in the armpits, groin, or anal area.
-
Significant pain and tenderness around the affected nodules.
-
Redness and visible inflammation in the impacted skin zones.
-
Persistent itching or a burning sensation on the skin.
-
Excessive sweating in the areas where lumps appear.
-
The development of thick or pitted scars over time.
The lumps caused by this condition may shrink on their own or rupture, releasing foul-smelling pus. In many cases, these nodules return after several weeks or months, often appearing in the exact same location as before.
It is common for people to mistake hidradenitis suppurativa for a standard boil. However, unlike common boils, the nodules from this condition often leave permanent scars on the skin.
Can hidradenitis suppurativa turn into cancer?
In rare instances, the chronic and recurring lesions associated with this condition can lead to the development of squamous cell skin cancer. This type of cancer begins in the outer layers of the skin and is typically triggered by long-term inflammation or chronic sun exposure.
What are the most affected body regions?
The areas most frequently affected by hidradenitis suppurativa are the groin, armpits, buttocks, and the region around the anus. However, it can also appear under the breasts, on the inner thighs, the scalp, or the torso.
How to confirm a diagnosis
A primary care physician or a dermatologist typically diagnoses hidradenitis suppurativa by physically examining the lesions and their location. Based on clinical guidelines from the American Academy of Dermatology, a healthcare provider will also evaluate your specific symptoms and review your personal and family medical history to ensure an accurate diagnosis.
Additional testing is rarely required to confirm a diagnosis. However, a doctor may perform a skin biopsy to rule out other conditions such as squamous cell carcinoma, lymphoma, or pyoderma gangrenosum, which is an inflammatory disease that causes skin tissue death.
Possible causes
Hidradenitis suppurativa occurs when a hair follicle becomes blocked and eventually ruptures. This release of keratin and bacteria into the skin triggers an inflammatory response, leading to the formation of painful nodules and pus.
Several factors can increase the risk of developing this condition, including:
-
Smoking or a history of tobacco use.
-
Being overweight or having obesity.
-
A family history of the disease.
-
Hormonal changes during puberty, menstruation, or menopause.
Environmental factors, such as the use of oral contraceptives, lithium, deodorants, or antiperspirants, have also been suggested as potential links. However, more research is needed to fully understand how these factors contribute to the development of the condition.
Treatment options
Treatment is focused on relieving pain, encouraging the healing of lesions, and reducing the frequency of flare-ups. According to the American Academy of Dermatology, a medical professional will tailor the clinical approach based on the severity of the symptoms, often combining topical treatments with systemic medications for more advanced stages
Commonly recommended treatments include:
-
Oral or topical antibiotics, such as tetracycline, rifampin, and clindamycin.
-
Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or acetaminophen to reduce pain and swelling.
-
Oral or injectable corticosteroids, such as prednisolone or triamcinolone.
-
Nerve pain medications, such as gabapentin or pregabalin, for chronic discomfort.
-
Anti-androgen hormone therapy, using medications like metformin, oral contraceptives, spironolactone, or finasteride.
-
Biologic immunosuppressants, such as adalimumab and infliximab, to regulate the immune system.
-
Surgery, which is usually reserved for severe cases that do not respond to medication.
Additionally, some patients may benefit from pulsed light therapy to help reduce inflammation in active lesions.
Doctors also recommend lifestyle changes to prevent the condition from worsening. These include laser hair removal, avoiding abrasive sponges or brushes on the skin, wearing loose-fitting clothing, maintaining a healthy weight, quitting smoking, and reducing the intake of high-carbohydrate foods.
Possible complications
Hidradenitis suppurativa can lead to various physical and emotional complications, such as:
-
Chronic pain.
-
Skin tightening that limits the movement of limbs.
-
Osteomyelitis (bone infection).
-
Severe systemic infections.
-
Recurrent cellulitis.
-
Permanent scarring.
-
Social isolation and depression.
-
Fistulas affecting the anus, bladder, or urethra.
In some cases, the condition is also linked to lymphedema, lymphoma, amyloidosis, anemia, or low protein and potassium levels in the blood.






























