Genital psoriasis is an autoimmune disease that affects the skin in the genital area. It presents with smooth, red patches that appear to be dry.
Genital psoriasis can affect both men and women and can develop in any part of the genital area, including the pubic area, thighs, buttocks, penis, or vulva.
Also recommended: Psoriasis: Symptoms, 10 Types, Causes & Treatment Options tuasaude.com/en/psoriasisAlthough it does not have cure, it is possible to manage genital psoriasis with the right treatment, prescribed by a dermatologist or immunologist.
Main symptoms
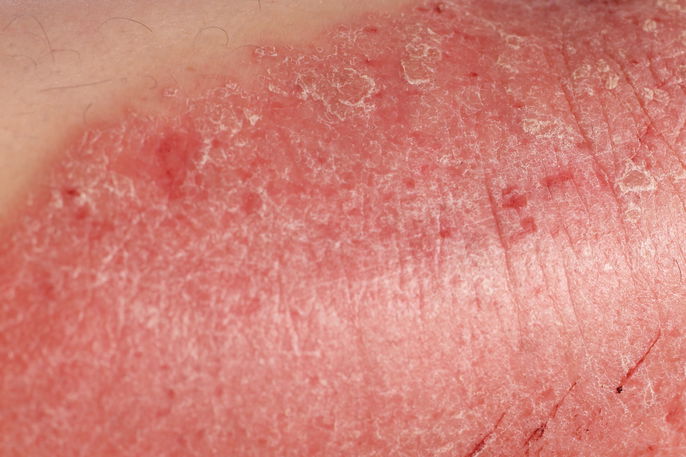
The most common symptoms of genital psoriasis include:
- Small smooth, red, and shiny patches in the genital area;
- Pain or discomfort in the affected area
- Intense itchiness in the area;
- Dry and irritated skin.
Symptoms of genital psoriasis are generally more common in people who are overweight. Symptoms tend to worsen with excessive sweating or prolonged use of hot, tight-fitting clothes.
Common causes
Genital psoriasis is an autoimmune disease that is characterized by healthy skin cells being attacked and damaged by immune cells. Skin cell damage will accelerates the cell renewal cycle, triggering skin cells to replicate very quickly. This can lead to inflammation and the formation of plaques that are characteristic of psoriasis.
Some factors can trigger or worsen genital psoriasis, such as a positive family history, stress, skin diseases, wearing tight clothing and being overweight.
Most affected areas
The most affected areas of genital psoriasis include:
- Pubis: affects the area above the genitalia where there is hair, and symptoms are similar to scalp psoriasis;
- Thighs: patches usually appear in the groin area, near the genitalia;
- Vulva: these patches are usually red and smooth and are only on the external part of the vagina;
- Penis: psoriasis usually occurs on the glans (head), but it can also affect the body of the penis;
- Buttocks and anus: the patches appear near the anus, causing intense itchiness;
- Armpits: symptoms get worse with tight-fitting clothes and sweat;
- Breasts: the patches usually appear in the bottom part of the breasts.
In men, genital psoriasis does not cause sexual dysfunction, however, the condition may cause anxiety which can interfere with intercourse. Also, some of the medications used for treatment can have side effects which can affect erection.
How to confirm the diagnosis
It is usually easy to diagnose genital psoriasis. A diagnosis is usually confirmed by a dermatologist following an assessment of the skin and the presenting symptoms.
The doctor may also order tests to rule out other causes for dry skin flare-ups, like bacterial or fungal swabs.
Treatment options
Genital psoriasis is usually treated with a topical corticosteroid cream which should only be used as prescribed over the affected area to decrease skin inflammation and relieve discomfort.
Also recommended: Psoriasis Diet Plan: Food to Eat & Avoid (w/ 3-Day Meal Plan) tuasaude.com/en/psoriasis-dietIn more serious cases, in which the patches do not improve with creams or when other body areas also get affected, the dermatologist may prescribe oral medication. Read more about the different psoriasis medication your doctor may consider prescribing for you.
Another alternative is UV light therapy, which consists of the application of UVA and UVB rays directly on the affected areas. This type of treatment is done in specialized dermatology clinics, and the duration and number of sessions depend on the skin type and the seriousness of the lesions.
These medical interventions can also be combined with home remedies for psoriasis, which can be prepared to help manage mild symptoms.
Tips for a quick recovery
The following tips will help with skin irritation and quick recovery after a flare-up:
- Wearing light, cotton clothes that are not tight-fitting;
- Avoid sweat in the area, and re-apply psoriasis cream immediately after showering or doing physical activity;
- Keep the affected area clean at all times;
- Avoid using perfume, soap, and creams not prescribed by a doctor;
- Avoid using perfumed panty liners or pads, as these can irritate the skin;
- Wash and remove prescription cream from your genital area before having intercourse;
- Wear a condom and lubricate the area well during intercourse;
- Wash your genitals after intercourse and reapply your prescription cream.
It's also important to remember that coal tar-based creams should only be applied in the genital area under doctor orientation, as using these in excess can make your skin more irritated and cause worsening flare-ups.






























