Nail disease can occur due to natural aging or from direct trauma to the nails. It can also occur due to a health condition, like a vitamin deficiency, hormonal changes, fungal infection, diabetes, heart disease, lung disease or even cancer.
Nail disease largely develops because most serious health problems affect oxygenation and interfere with how nails grow. These diseases can lead to color or shape changes, which require medical attention.
Healthy nails will generally be clear throughout and have a pink base. If you notice changes to your fingernails, you should see a family doctor or a dermatologist for testing, diagnosis and treatment as necessary.
1. Dry, breaking nails
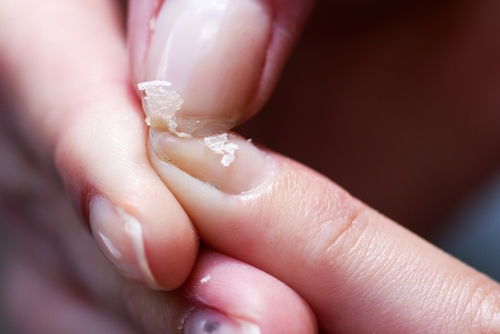
Dry and breaking nails will easily flake off or break, and usually are a consequence of normal aching. They can also occur due to chemical allergies (from detergents, soaps or cleaning products), from gel nail removal or from too many manicures.
This change may be sign of an iron deficiency, folic acid deficiency, vitamin A deficiency, vitamin B12 deficiency or vitamin C deficiency. These nutrients are necessary for the production of the protein that strengthens nails. Dry and breaking nails can also occur with health conditions like psoriasis, mycosis, hyperthyroidism or anemia.
What to do: You should avoid using products that may cause allergy to allow the nail to regrow. You should also avoid any manicures for at least 2 weeks. If the nails continue to be dry, you should see a dermatologist to determine whether it is related to a vitamin deficiency or another health condition.
2. Nails with white spots
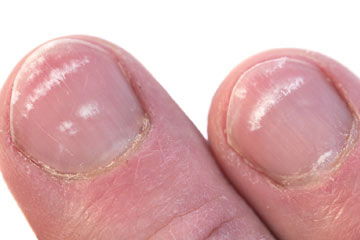
White spots on the nail, also known as leukonychia, usually happens to trauma to the nails (from a blow, hitting the nail on a wall, or getting a finger stuck in a car door). These white spots can also emerge due to hormonal changes throughout the menstrual cycle.
Generally, these spots do not indicate any health problems, but can also be a sign of antibiotic use or a health condition like vitiligo or hanseniasis.
What to do: You should also the nail to grow out naturally until the white spots disappear. If the white spots persist for many weeks, you should see a dermatologist for further assessment.
3. Yellow nails
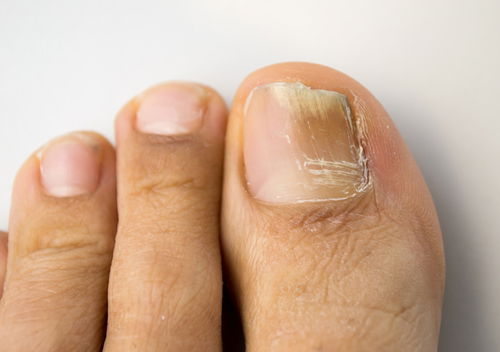
Yellow nails are common in older adults, in which case they are not a sign of any health condition. This coloring can also occur with medication use (like antibiotics), from contact with cleaning problems or from cigarette smoke. Excessive consumption of carrots, pumpkin or sweet potato can also lead to more yellow nails.
Yellow nails can also emerge due to a fungal nail infection, or from a health condition like diabetes, psoriasis, rheumatoid arthritis, liver disease (like cirrhosis or hepatitis) or lung problem (like COPD or bronchitis).
What to do: You should consult a dermatologist to evaluate the presence of a fungal infection or psoriasis, so that appropriate treatment can be initiated. If you suspect you may have another disease, you should consult a family doctor or can complete an initial evlauation and forward your case to other specialties if needed.
4. Blue nails

Blue nails can occur due to a low oxygen levels or lack of oxygen, which can cause the cuticle or membrane beneath the nail purple or blue. This condition is referred to as cyanosis, and is a common symptom of being in a cold environment. Blue nails can also occur with circulatory diseases (like Raynaud's disease), respiratory problems (like emphysema, asthma or pneumonia), or heart disease (like cardiac failure).
What to do: You should use gloves and move to a warmer environment if your blue nails are related to a cold environment. If you frequently notice blue nails, if they take a long time to revert to normal coloring, or if you have other symptoms like shortness of breath or fatigue, you should see a doctor for further assessment and treatment.
5. Red nails
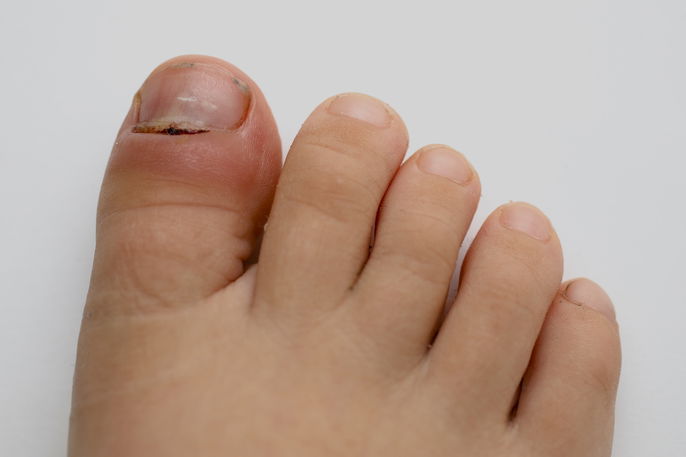
Red nails, particularly when they are red around the corners, usually occur due to a condition called paronychia. This can occur due to an inflammation caused by bacteria, viruses or fungi, from cuticle removal, fingernail trauma or an ingrown nail. In some cases, pus may start to develop around the nails.
Health conditions, like heart disease, lung disease, high blood pressure, or stroke, can lead to completely red nails.
What to do: You should consult a dermatologist if the nail is red around the borders. The doctor may order antibiotics or opt to drain the pus. If your nails are totally red, you should see a doctor immediately or proceed to the closest hospital for rapid treatment.
6. Green nails
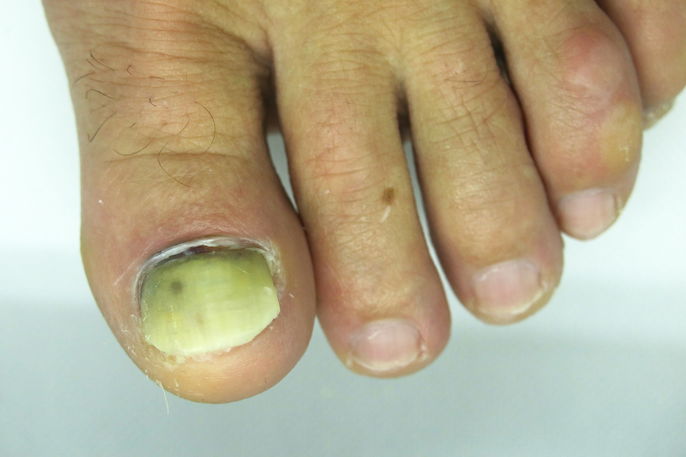
Green nails, also known as green nail syndrome, can occur due to an infection. It usually leads to green-blue or dark green coloring, and is caused by Pseudomonas aeruginosa bacteria.
This condition can emerge on the fingernails or toenails and is generally not associated with any pain. However, some people may experience swelling, discomfort or redness.
What to do: You should consult a dermatologist to start treatment with antibiotics to eliminate the bacteria.
7. Nails with dark lines
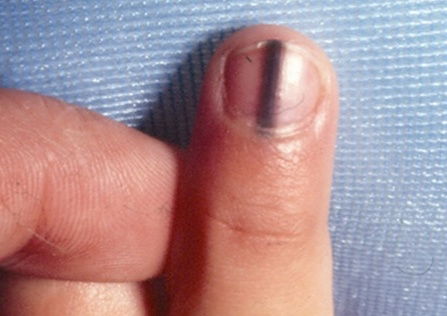
Nails with dark lines are caused by condition scientifically referred to melanonychia. It is more common in people with darker skin, but it can also emerge suddenly from medication use (antibiotics or zidovudine use, which is a medication used for HIV treatment).
These dark lines can give the nail a brown, gray or black appearance, which are noted from the base of the finger or toenail to the top. When these lines develop overtime, it can be a sign of increased melanin production, which can be one of the first signs of melanoma.
If you notice totally dark toenails, it can be a sign of a toe injury from tight shoes, a direct blow or from getting the toe stuck in an object. This can lead to bleeding and a dark toenail, as well as pain and discomfort.
What to do: You should consult a dermatologist to evaluate the cause of the dark lines on the nails. If it is related to a medication, the doctor may consider swapping it for another. Dark spots that develop over time and change color, size or shape should be assessed by a doctor to rule out melanoma.
A dark nail caused by an injury does not require any specific treatment, as the blood will naturally be absorbed as the nail grows.
8. Wavy nails
Wavy or rough nails can occur from normal aging and are common in older adults. They can also develop due to skin conditions that dry out the skin, like psoriasis, lichen planus, atopic dermatitis, alopecia areata or lupus.
What to do: You should consult a dermatologist for the most appropriate treatment.
9. Bubble nails
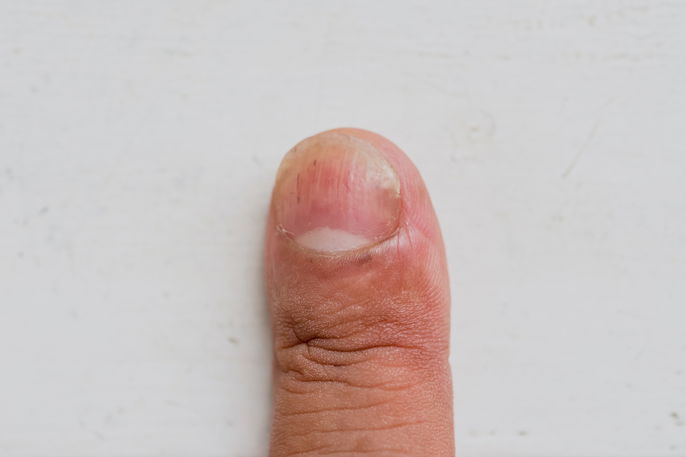
Rounded or bubble nails can start gradually and develop over several years before becoming noticeable. It can worsen with time, and nails can become swollen and uncomfortable when pressed.
This condition may be a consequence of low oxygen levels from lung or heart disease, but it can also occur with liver disease, inflammatory bowel disease or HIV infection.
What to do: You should consult a family doctor for assessment and testing. Depending on the underlying disease, the doctor may refer you to a cardiologist, gastroenterologist or infectious disease specialist for treatment.
10. Spoon nails
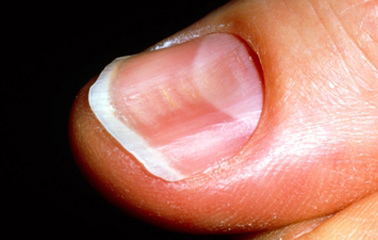
Spoon nails, or koilonychia, is a condition in which the fingernails curl up on the ends, giving them a spoon appearance. This is usually sign of poor circulation to the center of the nail, which can happen with an iron deficiency, cardiac problem or hypothyroidism.
What to do: You should consult a dermatologist or family doctor for testing to rule out a thyroid or heart problem, or a nutritional deficiency.
11. Nail separation
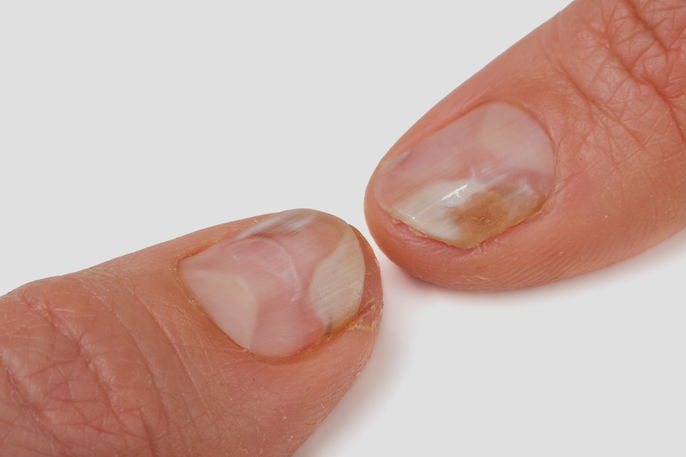
Nail separation, or onycholysis is characterized by total or partial separation of the finger or toenail for the nail bed. It can occur with tight shoes, excessive nail grooming or allergies to cleaning products.
This condition may also be caused by a fungal infection, psoriasis or hyperthyroidism, as well as medications like captopril or retinoids.
What to do: You should avoid using tight shoes and avoid cleaning beneath the fingernails constantly. You should use gloves to avoid direct contact with chemicals and cleaning products. If the nail separation does not resolve on its own, you should consult a dermatologist for diagnosis and treatment.






























