- Milia are small white or yellow bumps caused by trapped keratin and are most common on the face.
- Milia are usually harmless, and they can look similar to other skin conditions such as acne, heat rash, or sebaceous hyperplasia.
- Milia in babies are very common and usually go away on their own.
Milia are small white or yellow bumps that form when keratin becomes trapped under the skin. These tiny cysts usually appear on the face, especially around the eyes, nose, and cheeks, but can also develop on other parts of the body.
Milia can be caused by factors such as sun damage, skin injuries, use of heavy or oil-based products, or natural skin healing. They are also common in newborns and typically do not cause pain, although mild itching may occur in some cases.
Treatment for milia may include simple skin care, topical retinoids, cryotherapy, or professional extraction by a dermatologist. There are also different types of milia depending on their cause, which may require specific approaches for proper diagnosis and management.
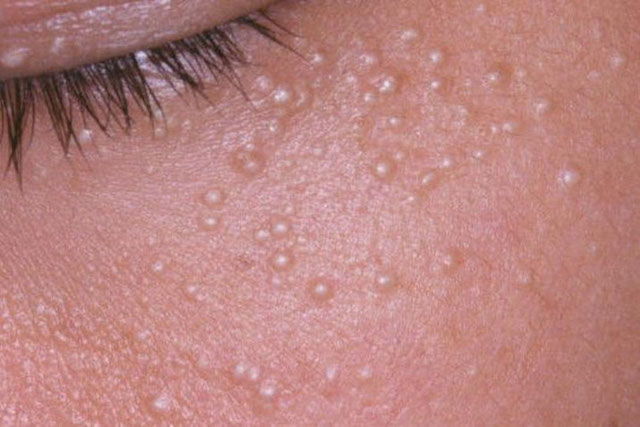
Main symptoms
The main sign of milia is the appearance of small white or yellowish bumps on the skin, usually measuring 1 to 3 mm. These bumps often appear close together and typically do not cause discomfort such as itching or pain.
Milia are most common on the face, particularly on the nose, forehead, cheeks, and eyelids. They may also appear in the genital area, such as on the labia majora in women or the glans in men.
Confirming a diagnosis
Milia are usually diagnosed by a dermatologist based on the person’s symptoms, medical history, and the appearance of the skin lesions during the examination.
To confirm the diagnosis, the dermatologist may also perform dermoscopy, an examination that uses a special magnifying device to observe the lesions in greater detail.
Possible causes
The main causes of milia include:
-
Accumulation of dead skin cells beneath the surface of the skin
-
Skin damage caused by burns or sun exposure
-
Healing of areas where blisters have formed
-
Use of certain medications, such as oral anti-inflammatory drugs or corticosteroid creams
-
Genetic or autoimmune conditions, including lupus or lichen planus
In most cases, milia form when dead skin cells are not shed through the skin’s natural exfoliation process. As new skin cells grow, the trapped dead cells can become enclosed beneath the surface, leading to the formation of small bumps or cysts.
Other skin conditions, such as miliaria, sebaceous hyperplasia, and acne, can also cause small bumps and may sometimes be mistaken for milia.
Main types
There are several types of milia, classified according to their cause and location. Some of the main types include:
- Neonatal milia: Occur in about half of newborns and are characterized by small skin cysts that disappear over time. They often appear on the nose, cheeks, or inside the mouth.
- Primary milia: Develop in adults and present as small, visible papules on the eyelids, cheeks, or forehead. In rare cases, they may appear in the genital area.
- Juvenile milia: Associated with genetic disorders such as Rombo syndrome, Gorlin syndrome, Bazex-Dupré-Christol syndrome, paronychia, and Gardner syndrome.
- Milia en plaque: Occur when multiple milia cysts form in the same area, creating an inflamed plaque on the skin. This type most often appears behind the ear or on the cheek.
- Traumatic milia: Develop in areas of the skin that are healing or scarred, often after burns or injuries that cause blistering.
Prolonged use of certain skin products, such as creams, ointments, petroleum-based cosmetics, lanolin, corticosteroids, or hydroquinone, can contribute to the development of milia.
Milia removal
Milia are not considered a serious condition and may sometimes disappear without specific treatment. However, if you would like to have them removed, it is best to consult a dermatologist, who can recommend the most suitable treatment for your situation.
The most commonly recommended options for treating or removing milia include:
1. Skin care
Following a consistent skin care routine that includes washing the skin with warm water, using an oil-control soap, and applying moisturizer and sunscreen regularly can help reduce existing milia and prevent new ones from forming.
2. Ointments
The doctor may prescribe ointments containing retinoids or retinoic acid to promote skin renewal and help remove the spots caused by milia. Learn more about tretinoin and how it is used.
3. Cryotherapy
Cryotherapy is a treatment that uses a cold substance to freeze and remove skin lesions. In some cases, this procedure may be recommended to remove a milium.
4. Milium extraction
In some cases, extraction may be indicated and performed by a dermatologist using a minor procedure. The doctor typically uses a fine needle and sterile instruments to safely remove the bumps.
According to the American Academy of Dermatology, milia should not be squeezed or removed at home, as this can damage the skin and increase the risk of scarring.
Milia in babies
According to the American Academy of Dermatology, milia are very common in newborns and typically clear up on their own without treatment.
In babies, milia often appear during the summer or on very hot days within the first few weeks of life. They may also occur when the baby has a fever.
When sweat cannot pass through the pores, particularly on areas like the nose or cheeks, small blister-like papules may form. These papules are usually filled with fluid and tend to rupture easily.






























